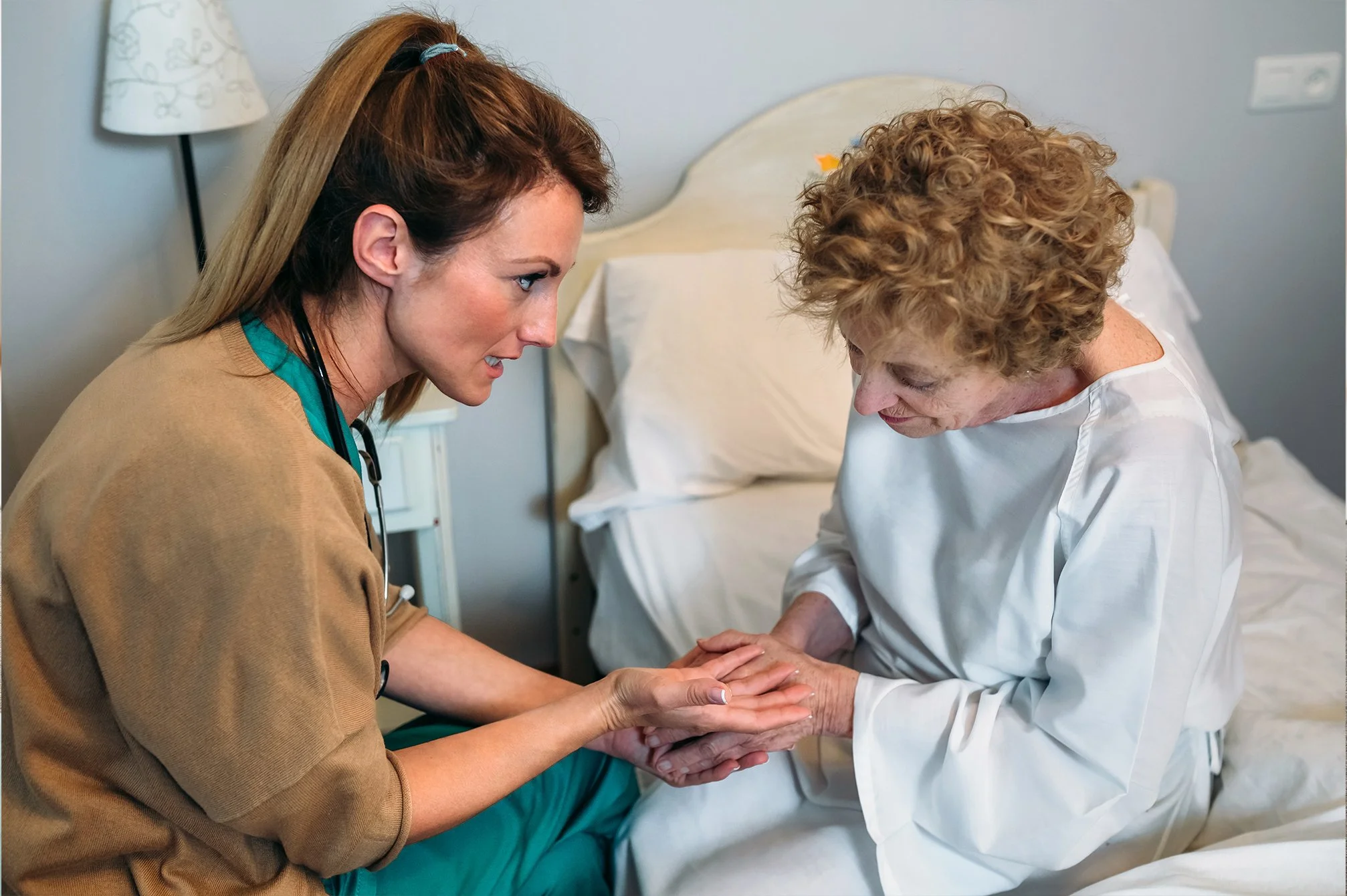
In a previous blog, I shared some information and tips about how Medicare covers (or doesn’t cover) preventive care. It was a good generalization related to Original Medicare as a whole. To take it a step further, let’s dive into preventive care and how it pertains to Advantage Plans or Part C. As a rule, if Original Medicare covers a medical service, then the Advantage Plan is required to cover it as well. There are, however, differences in cost share, authorization processes and how the covered service is billed and paid. In addition, one could argue that Advantage Plans go beyond Original Medicare in covering preventive services. Let’s look at how that plays out.
Medicare and Preventive Care—Is This Bill Real?
On more than one occasion, I have received a call from a client fairly new to Medicare concerned about a bill. In one case, a client went for an annual physical at his Family Doctor’s office and was shocked to find his visit was not covered by Medicare. In addition, he stated his doctor recommended a Tetanus booster shot since he hadn’t had one in over ten years. He later got a bill for over $300. So how can this be and what, if any, preventive care does Medicare cover? Here is a look at what is covered and what to look for if you get an unexpected bill!
Late Enrollment Penalties—I’ve Got Them, Now What
I wrote and posted a previous blog on what Late Enrollment Penalties are and how to avoid them. [https://www.cdi-cares.com/blog/what-are-medicare-penalties-and-how-do-i-avoid-them] But let’s go a bit further to help Medicare beneficiaries who already have Late Enrollment Penalties (LEP). I have found that some clients come to me after the fact and don’t even realize they have a Late Enrollment Penalty (LEP). Also, once you are notified that you have a penalty, how do you pay it? Is there anything you can do about it after the fact? Let’s get into it!
Prior Authorizations Will My Procedure Be Denied?
When deciding whether to use Original Medicare with a Supplement Plan as primary coverage versus enrolling in an Advantage Plan, the growing concern many have is with Prior Authorizations. There has been a lot of chatter and negative attention in the media about Medicare beneficiaries being denied medical care by insurance companies. So, is this true? Should you be concerned? I think it is helpful to first understand what a Prior Authorization is for and how it came about. Then, I’ll share how to navigate that process to get what you need out of your plan. Let’s go…..
What’s Coming in 2024…..
Each year as we head toward the last quarter of the year, the Center for Medicare/Medicaid Services or ‘CMS’ begins to announce changes to Medicare for the coming year. Sometimes the changes are new regulations put in place by CMS, and sometimes there are changes written and signed into law by the acting government. So, what is coming up for 2024? Here is a sneak peak at the exciting and maybe not so exciting changes.
What is Post Acute Care
Most of us understand how Medicare works and pays for a hospitalization and going to the Doctor’s office for visits. We even have a pretty good understanding of how to use our insurance to get labs drawn, x-rays, MRIs or go to the ER. What can sometimes be confusing is how Medicare works in areas of Post Acute Care. As we age and/or have multiple complicated conditions, we may need ongoing care after a serious illness, surgery or hospital stay. Post Acute Care encompasses home health care, home or outpatient therapy, hospice care or skilled rehabilitation. Let’s take a deeper dive into those services and what to expect in terms of Medicare coverage.
SSA Medicare Tips and Tricks
HOW TO AVOID STANDING IN LINE
When the pandemic hit, all government offices shut down to anyone in person needing assistance. This left Seniors at a major disadvantage. Seniors are the largest group of people that rely on the Social Security Administration for enrolling in retirement benefits and their medical benefits. Everything had to be done over the phone with long hold times or online. No one enjoys these processes, let alone the generation who did not grow up in the high-tech world we see today. This is when I took a deep dive and learned all the tips and tricks on how to navigate the Medicare world without walking into an SSA office. Here are some valuable tips I picked up….
Medicare Alphabet Soup–The Difference Between Plan G and N
The first distinction to make here is that Plan G and Plan N are types of Medicare Supplement or Medigap Plans. In other words, these are not Advantage Plans (Part C) or Prescription Drug Plans (PDP). Medicare loves using letters to name benefit options and plans, which often makes the whole thing more confusing. Acronyms are another favorite as in MA Only, MAPD, DSNP, HMO, PPO, etc. We can address that another day! But not to worry, CDI is here for you! In this blog, I want to help highlight the difference in these two supplement plans which are currently the most popular and beneficial among the supplement offerings [as of 2023].